*Individual results may vary
What is Labiaplasty?
Labiaplasty, or vaginal rejuvenation, is a surgical procedure that is performed on the vaginal labia (lips). This procedure could focus on either the labia majora (the outer vaginal lips), the labia minora (the inner vaginal lips), or both. It is performed to reshape uneven labia and to reduce the size of too large labia. Women who are looking to improve the appearance of their labia, address discomfort during intercourse (dyspareunia) due to the excess labia being pulled upon, improve their hygiene, or to relieve pain and irritation are often good candidates for this procedure.
Am I A Good Candidate for Vaginal Rejuvenation?
There are many reasons why a woman would want to consider undergoing labiaplasty. Typically, women who do not like the appearance of their vaginal lips make good candidates for this procedure. Additionally, women who experience labial irritation during normal activities, find it difficult to keep clean, or experience pain during intercourse may also want to consider labiaplasty as a solution. To be considered to this procedure, potential candidates should be:
- In relatively good health for surgery
- Non-smokers
- Concerned or self-conscious about the appearance of your labia
- Discomfort during intercourse due to pulling of the labia
- Irritation in clothing from excessively large labia
- Difficulty with personal hygiene due to the excess amount of labia
- Discomfort during certain activities (ie bicycle, horseback, exercycle, motorcycle) due to the excess labia
- Failed or unsatisfactory previous labiaplasty – these can often be improved with revision surgery.
- A thorough examination during your consultation demonstrates that you are an ideal candidate for this procedure
What Are The Benefits of Labiaplasty Surgery?
Deciding to undergo labiaplasty is a very personal choice for many women. There is an extremely high rate of satisfaction and improvement in self-esteem following labiaplasty. Benefits of labiaplasty include:
- Relieving pain during intercourse
- Reducing irritation during normal activities
- Rejuvenating labia after weight loss or aging
- Restoring labia after childbirth
- Reducing larger labia
- Restoring self-confidence
The benefits of labiaplasty are not strictly aesthetic. Many women experience daily pain and discomfort due to their uneven or larger labia, as well as reduced pleasure during intimacy due to discomfort and feeling self-conscious about their appearance.
3D Imaging in Labiaplasty Surgery
I have been using three-dimensional (3D) imaging for both the preoperative planning of surgery as well as to show and compare the before and after surgical results. This technology affords a better understanding of the anatomy of the female genitalia both before and after surgical intervention. It allows one to better appreciate the magnitude of the physical change to the contours of the entire vulva. The three-dimensional images can freely rotate about in space to facilitate a thorough analysis of the changes to be made surgically. They also help to document the progress achieved after surgery. The below video demonstrates how I use this exciting new technology.
Anatomical Considerations in Vaginal Rejuvenation
There are two sets of female genital “lips”. The outer lips, or labia majora, are thick skin folds that comprise the outer border of the female genitalia. They are of variable length, but even when on the longer side, they still only measure no more than 2 cm or so. The labia majora are thick, and as such, are not very movable. The inner lips, or labia minora, are much thinner than the outer lips. They lie between the outer labia majora lips and to either side of the border of the vaginal orifice (opening). This is depicted in Figure 1.
The labia minora is a sheet of tissue comprised of three layers. Plywood is a sheet of wood comprised of about eight layers. Same idea. The outer layer of the labia minora is comprised of epidermis (dry skin). The inner layer is comprised of vaginal mucosa quickly transitioning to epidermal skin as you move away from the vaginal opening towards the outer edge of the lip (towards the thigh). The intervening tissue between these layers is fibrous connective tissue (no fat) only a couple of millimeters thick. This tissue is very important to the success of the labiaplasty procedure. The length of the labia minora, from vaginal opening towards the thigh, is very variable. Sometimes the length can be up to 4 or 5 centimeters (about 2 inches), occasionally even longer.
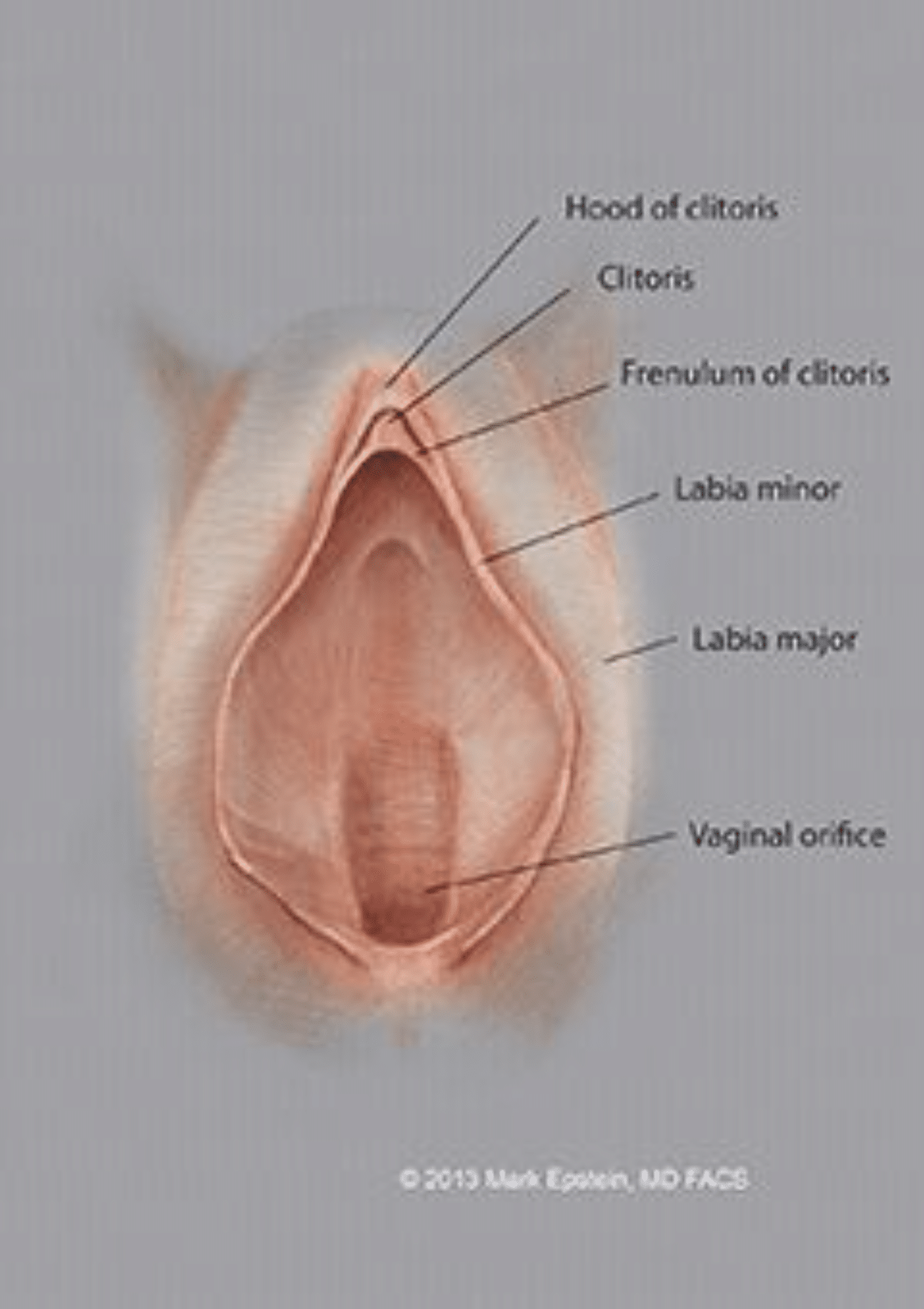
Figure 1: Diagram of the external anatomy of the vulva demonstrating the relationship between the labia major and labia minor, the clitoris and its “hood” and the vaginal orifice (opening).
In most women, when standing, the labia minora are either flush (even) with the labia majora or even receded back behind the labia majora and not visible from view. When the labia minora are lengthened, they protrude past the labia majora and sometimes hang downward. My patients frequently express to me that they wish to have the labia minora not visible when standing. This is one of the goals of my labiaplasty procedures.
The Problem in a Nutshell
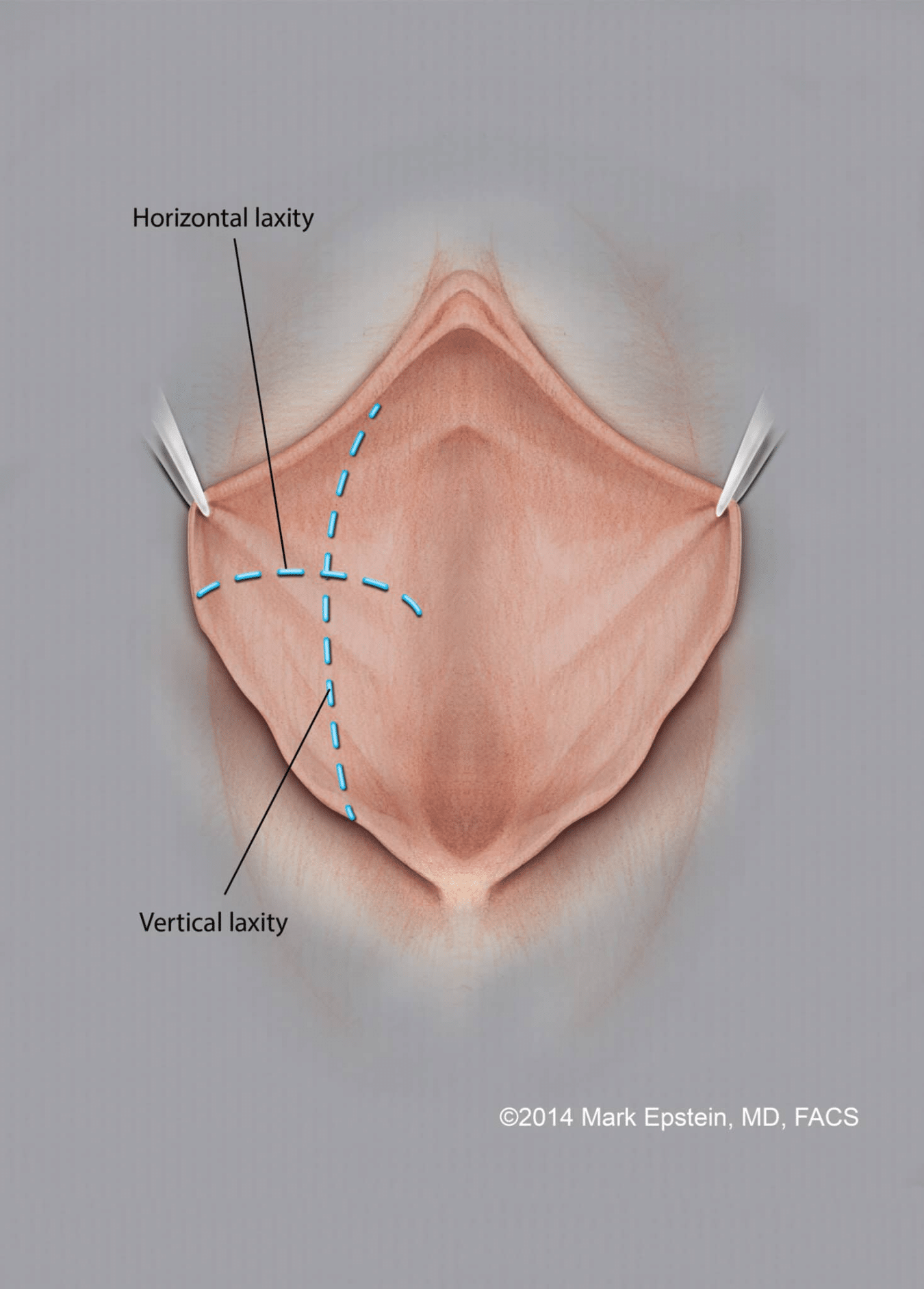
In the diagram on the left, there is an enlarged labia. The enlargement extends horizontally, towards the thighs when the skin is pulled away from the vagina. There is also excess running vertically, extending from the top of the vulvar cleft (the point where the top of the right and left labia minora come together in the midline) to the perineum (the point where the bottom of the right and left labia minora come together, near the anus). Tissue needs to be removed from the labia in such a way that the horizontal excess and the vertical excess are both reduced, or the aesthetic result of the procedure will be poor. The clitoral hood is an entirely separate issue but can be dealt with simultaneous to the labiaplasty.
Does a Labiaplasty require anesthesia?
Labiaplasty performed awake or asleep – Your choice!
Labiaplasty is easily performed under either general anesthesia or local anesthesia with ProNox®. Local anesthesia is actually a nice option for those that do not mind being awake during the surgery. The only discomfort is during the 10-15 seconds it takes to inject the local anesthetic. The ProNox® does a very nice job of relaxing you reducing the discomfort of the injection. After the local anesthetic is in, you will feel absolutely nothing. After the excess tissue is removed, the skin is closed with an absorbable suture, so no suture removal is required. Discharge home when using a local anesthetic is usually fifteen minutes after completion of the surgery, about 45 – 60 minutes after general anesthesia.
How long does a Labiaplasty procedure take?
The procedure takes about 75 – 90 minutes.
How is Labiaplasty performed? – Different Surgical Options
There are several ways to perform labiaplasty. The first is simply trimming the external excess labial skin also known as the lateral trimming technique, however, there are more sophisticated techniques such as the central wedge resection or “V” resection and the custom flask labiaplasty techniques. Below I explain all of these techniques in great detail.
VIEW OUR
Photo Gallery
The “Lateral Trimming” Technique
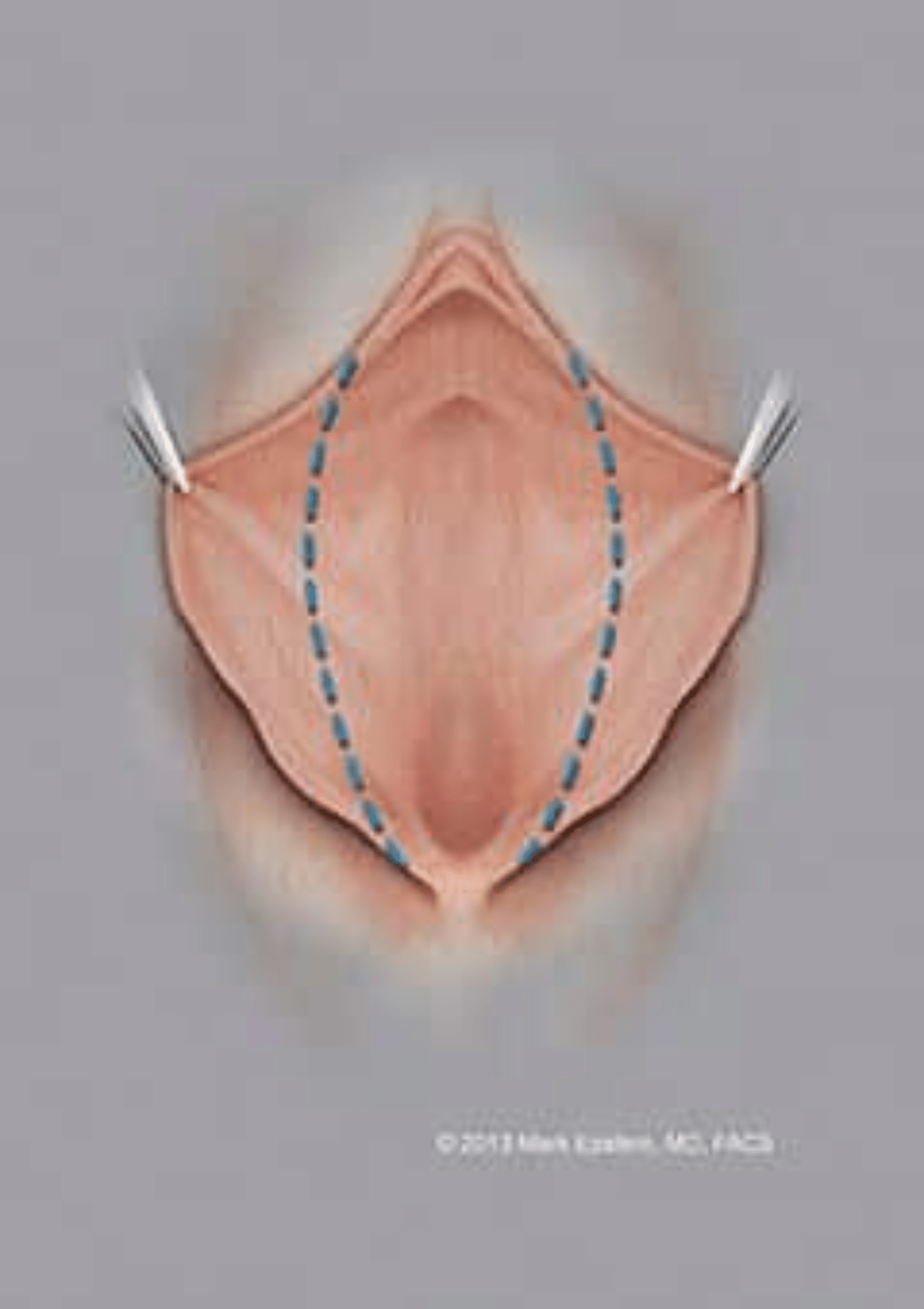
Figure 2: The resection of excess skin is marked along the labia.
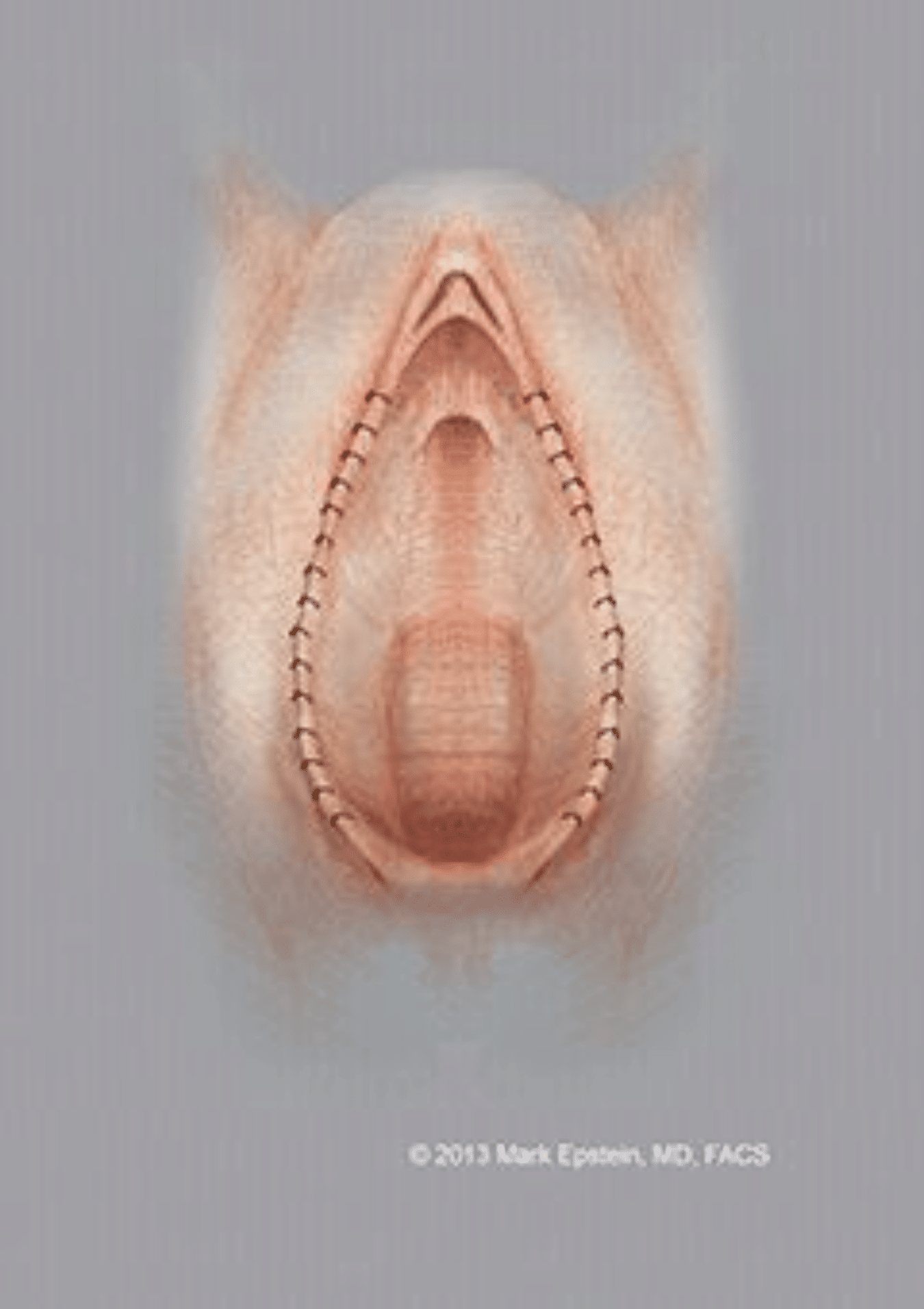
Figure 3: The excess labial skin has been removed and the raw tissue edge along the labial edge is sutured. The final result is shown.
Probably the most commonly performed, as well as the easiest technique is to simply trim the excess labial skin. The advantage of this procedure is that it is simple to understand and technically easy to perform. It will not address excess clitoral hood skin. One disadvantage to this method is that the normal outer border of labial skin is removed and a new edge of skin is created as the three layers of labial skin (the inside and outside skin, middle layer connective tissue) heal together.
Sometimes, there can be an irregular, almost “sawtooth” contour to the edge of the skin as it heals. This can happen when there is a lot of swelling after the surgery and the sutures placed into the edges of the skin cut into the skin edge as the swelling progresses. I have seen this happen on one occasion however it was successfully corrected by surgical revision.
The other disadvantage is that this procedure does not do a very good job of holding the edge of the labia minora within the confines of the labia majora. As stated earlier, it is desirable to have the labia minora set back so as not to protrude any further than the outer edge of the labia majora. Although the lateral trimming technique will reduce the size of the labia in width, it does not reduce the height of the labia. This vertical laxity will result in the labia minora protruding forward in some cases, despite the fact that it was trimmed horizontally, or “front to back”. Ideally, the labia minora needs to be under some degree of tension to prevent such “bowstringing” forward. Think of the labia minora as you would a violin string – if the string is under proper tension, it stays close to the fingerboard of the violin, but if the strings are loose, they will bow forward.
The other two techniques do a much better job of holding the labia minora back, at least in my opinion. Lastly but infrequently, the outer edge of the labia minora can be a source of some discomfort to the patient, although I have not personally heard this particular complaint from my patients. Despite the disadvantages stated, I have seen a high degree of patient satisfaction in my patients using the lateral trimming technique. For most patients, I prefer the other two procedures because I believe that the results are significantly better.
The “Central Wedge” Resection Technique
(Preferred in most cases)
The “Central Wedge” resection, devised by my colleague Gary Alter, M.D., is a bit more difficult to understand conceptually, however, it is really not that complicated. In this technique, a wedge of excess labial skin is removed, but the pattern of excision is a little different on the inside aspect of the labia as compared to the outside of the labia. On the inside, it is more of a “V turned sideways” pattern, and on the outside, it is more of a “V turned upside down” pattern.
There are several distinct advantages to this technique. First, the natural edge of the labia is preserved throughout. The second is that the apex of the outside “V” (the top of the excision) can be taken all the way up to the level of the top of the clitoral hood so as to remove excess clitoral hood skin when it exists on the outside of the hood, which is very common. (Excess inner clitoral hood skin is less common and can be addressed by simple excision of that skin separately). If you simply trim the excess labial skin along its perimeter (the first technique) and there exists excess lateral hood skin, this lateral hood skin will not be able to be addressed and will look like a strange blob of wrinkled skin on top of the clitoris. Excess labial tissue can be removed both horizontally and vertically with the Central Wedge technique.
Using the Central Wedge technique, this excess clitoral hood skin can be seamlessly incorporated into the outside labial skin excision and the results will look absolutely beautiful*! If the clitoral hood needs to be elevated as well, a separate set of incisions is usually required (discussed below). The results of the central wedge resection and clitoral hood reduction will flow seamlessly together.
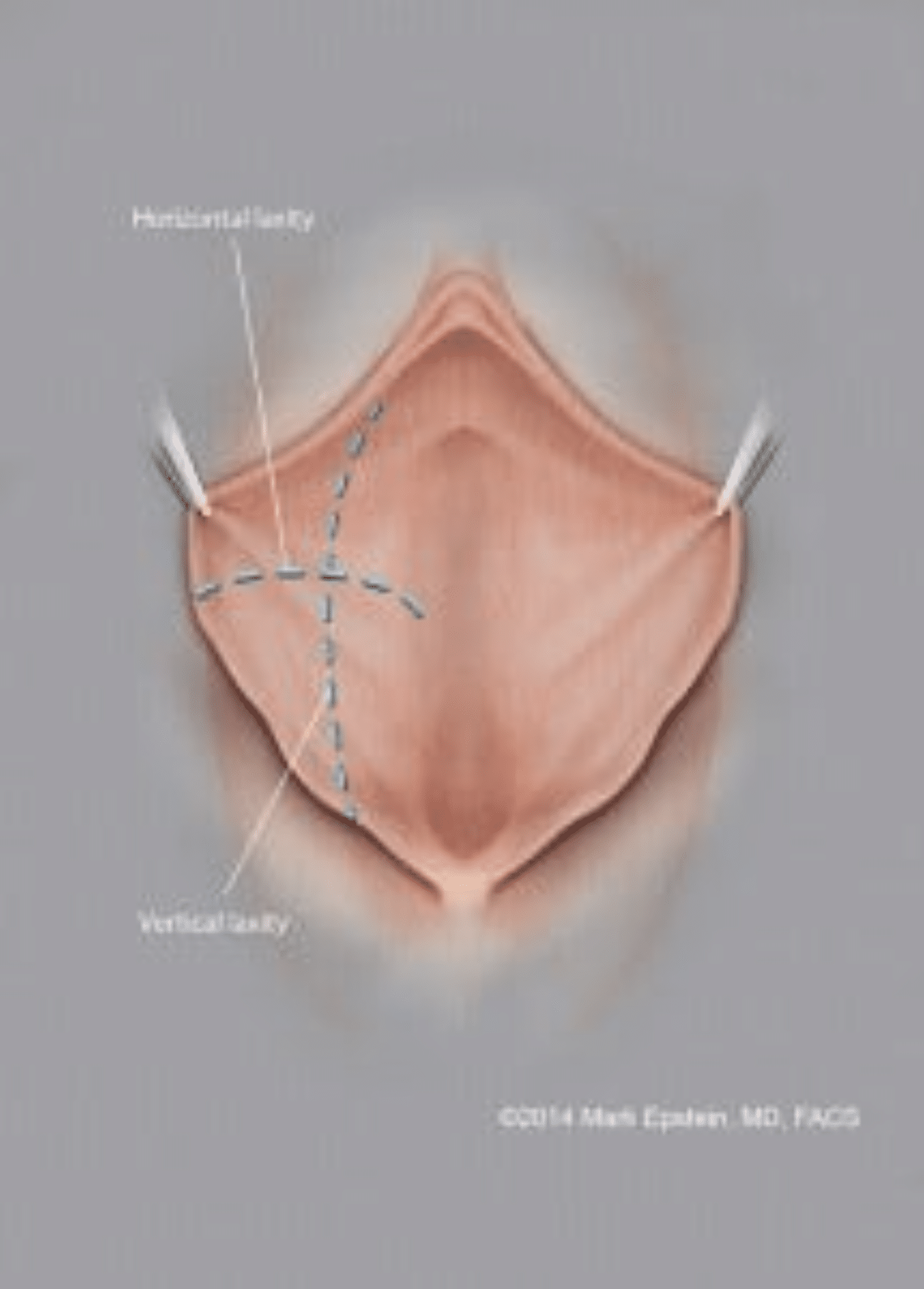
Figure 4: Labia minora showing excess tissue both horizontally and vertically. If the vertical excess is not addressed, the labia will often extend outside the confines of the labia majora, despite a reduction in horizontal excess.
The disadvantages of the Central Wedge technique are relatively minor: occasionally there is a more distinct transition of pigmentation between the upper and lower portions of the labia at the suture line, but this tends to lessen with time. Also, if there is a breakdown in the suture line, there can be a small hole within the scar, almost as if there was a small piercing placed there. This happens fairly uncommonly. It is referred to as a “fistula” and is easily repaired*.
The main advantage of the Central Wedge technique is the quality of the aesthetic result. The ability to obtain a natural looking result without excess labial skin which could be a source of cosmetic concern, or pulled inside the vagina during intercourse or irritated by clothing. This technique is now my preferred technique in most cases and even in revision cases.
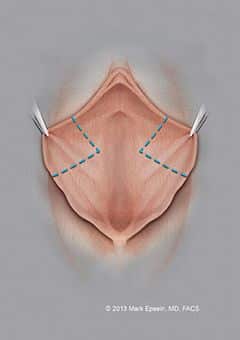
Figure 5: The incisions are somewhat different on the inner and outer aspects of the labia. In this figure, on the inner aspect of the labia, the “central wedge” or “V” is shown with the apex of the “V” pointing into the vagina (but not entering it). The mucosa, but not the tissue between the inner and outer layer of the labia is removed as shown.
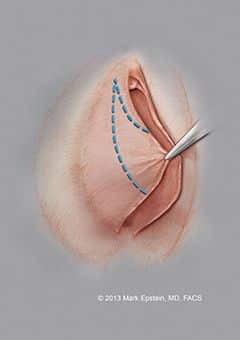
Figure 6: The incision on the outer layer of the labia is shown. If there is excess lateral clitoral hooding, resection of this excess hood skin can be incorporated into the design of the resection of skin. Again, only the skin, and not the tissue between the inner and outer layer of the labia is removed as shown.
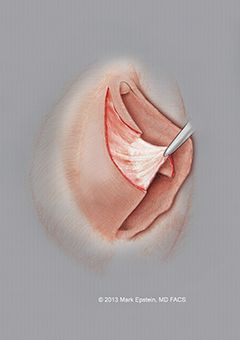
Figure 7: The resection of excess skin is complete. Now the incisions in the labia must be closed.
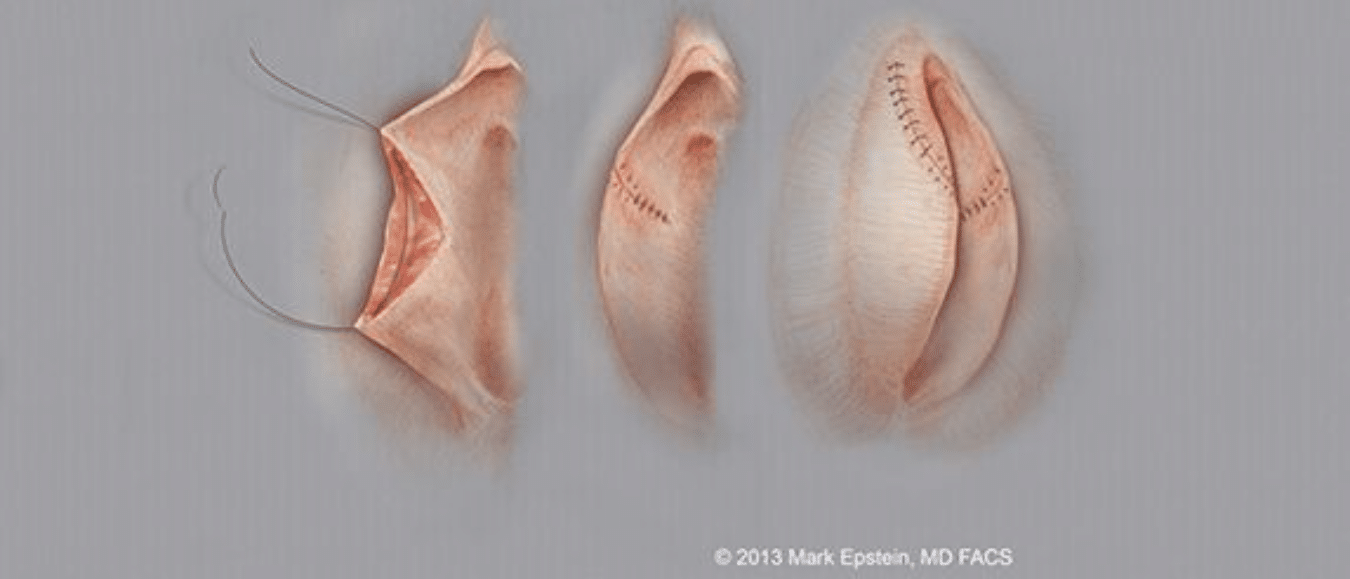
Figure 8: First, the tissue between the inner and outer layers of the labia is closed, followed by the inner and outer layers of the labia. Two different suture techniques are used to secure the repair and prevent wound separation. The final result is shown.
The “Custom Flask” Resection Technique
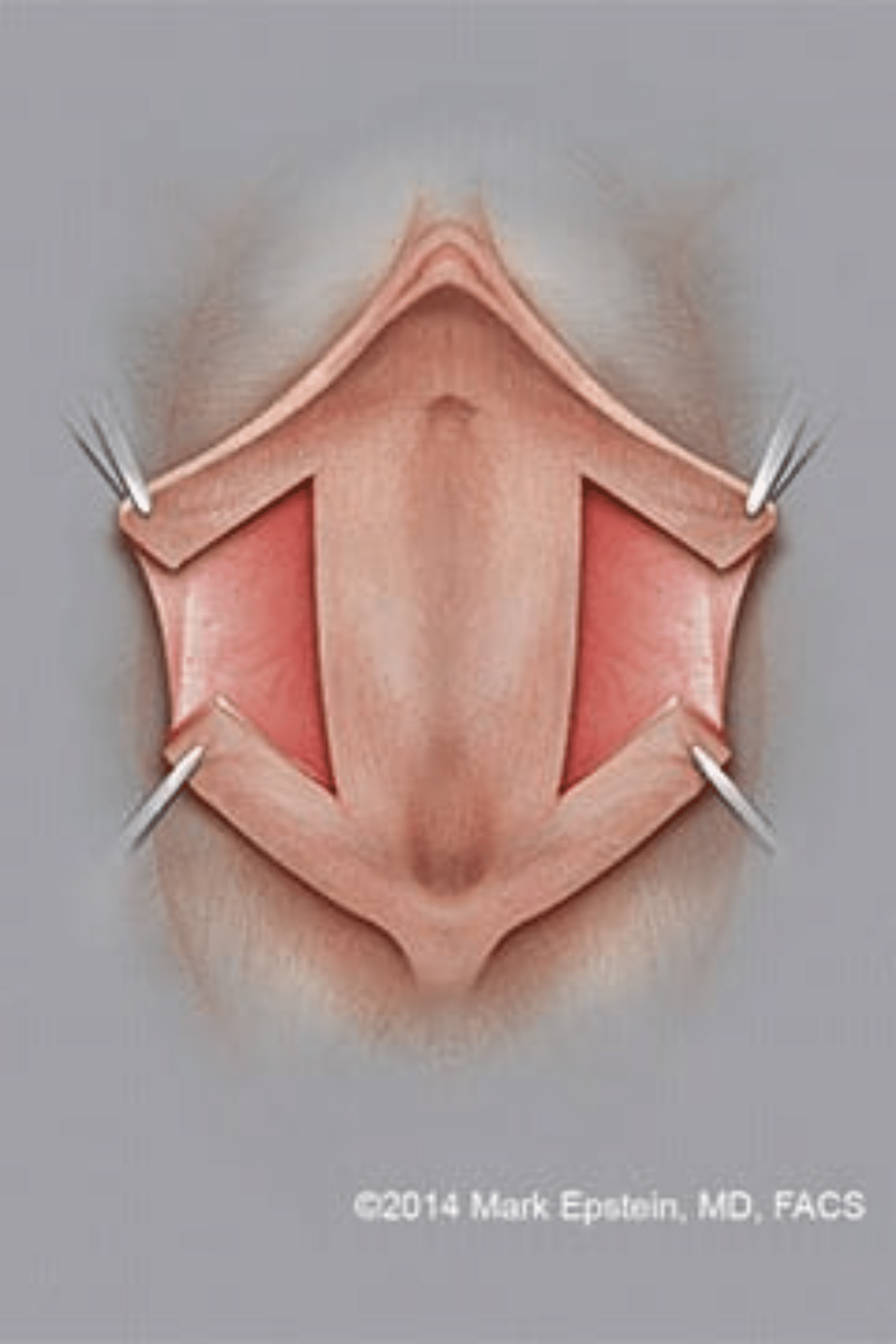
Figure 9: The incisions are marked for the Custom Flask labiaplasty. The pattern of skin to be removed resembles that of a laboratory flask, hence its name.
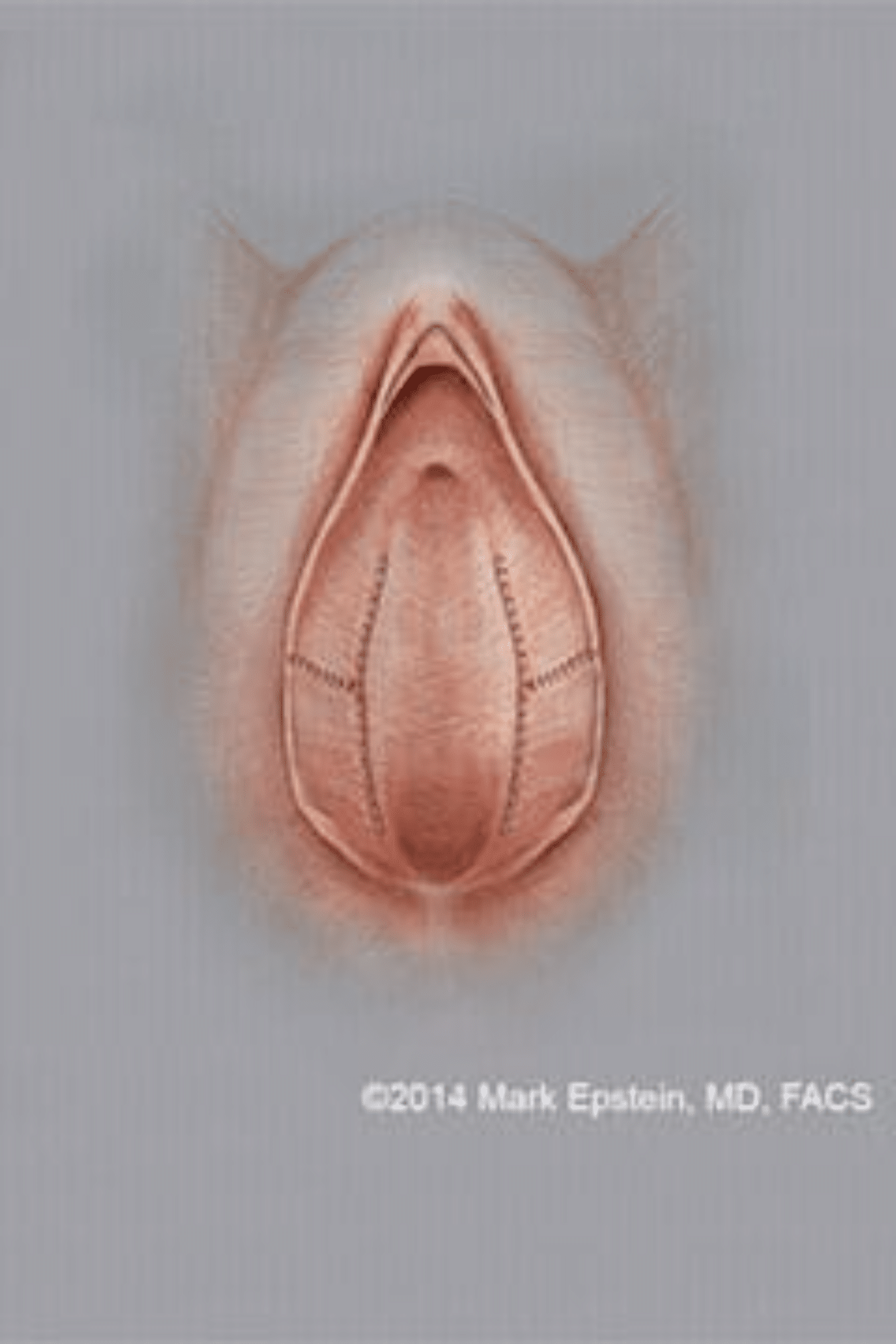
Figure 10: Final closure. The upper and lower outer limbs are brought together. The two are then attached to the outer edge of the vaginal opening.
The Custom Flask Resection, described by another colleague, Federico Gonzalez, M.D., will pretty much yield a nice result on any case that the Central Wedge technique will be applicable. One disadvantage is that the Custom Flask resection will not by itself address excess clitoral hood skin. A separate set of incisions needs to be made for removal of excess clitoral hood skin and clitoral hood elevation (if necessary). This is a very simple procedure and I would not consider this a decision factor against the Custom Flask labiaplasty.
What I love about the Custom Flask labiaplasty is that it is (in my opinion) the procedure of choice when a patient presents with a substantial amount of labia minora skin AND a narrow vaginal introitus (opening) as in a woman who is a still a virgin. The problem in this case with a Central Wedge resection is that a large sidewards “V” of labia minora tissue needs to be removed. That will require the vertex (lower point) of the “V” to be well into the vaginal canal. This can result in a significant narrowing of the vagina, making intercourse problematic. I also prefer this technique in woman who suffer from vaginal spasms, and those who have labia minora with a very broad base, beginning at the top of the labia and extending to the bottom of the labia, as opposed to a narrow excess of tissue.
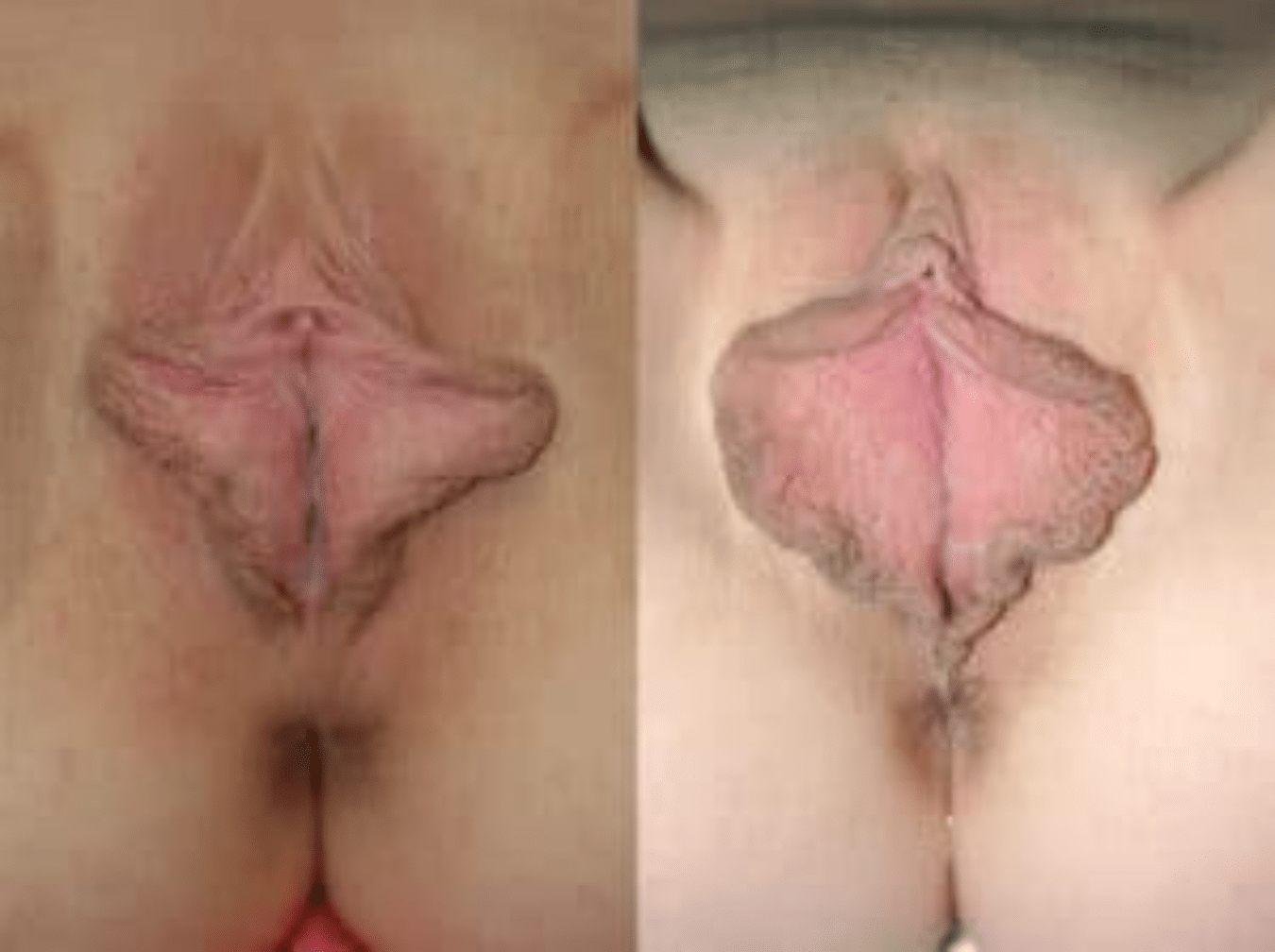
Both of the above patients possess a horizontal and vertical excess of labial tissue. However, the shape of the labia minora vary considerably. The patient on the left has a narrow “tongue” of excess labial tissue. This is very amenable to a wedge resection and such can be performed with very little extension into the vagina. The patient on the right has a labia with a much broader shape, beginning from the very top to the very bottom of the labia minora. A wedge resection in this case would result in the wedge extending far into the vagina with concerns about causing narrowing. This patient also is a teenager and a virgin, so such a resection would almost certainly cause substantial vaginal stenosis (narrowing), making intercourse difficult, if not impossible. You can view the entire case for the patient on the right here, and the patient on the right here.
The Custom Flask resection does not require any incision into the vaginal introitus itself. It yields a nice reduction of tissue and keeps the labia minora under proper tension so as to hold the edge of it within the confines of the labia majora. It is also simple to perform. A clitoral hood reduction/elevation can easily be performed concurrently. When healed, the results of this technique look essentially identical to that of the Central Wedge technique, except the suture lines, which are nearly impossible to see, are in different places. In summary, the cosmetic results of the Central Wedge and Custom Flask Resection techniques are in my opinion, identical.
Comparison of Labiaplasty Techniques
Historically speaking, I began my labiaplasty experience by performing the lateral trimming technique. As of several years ago, I have discontinued this procedure in favor of the central wedge and custom flask labiaplasty techniques. At the current time, I cannot think of a single reason to perform the lateral trimming technique over the other two.
What I do not like about the lateral trimming technique for Labiaplasty:
- Addresses only horizontal excess of labia tissue, not vertical excess (discussed below).
- The edge of the labia is composed of scar tissue, not normal labial edge.
- Occasionally has scalloped (irregular) edges which does not happen with the other two techniques. This is a known risk of the lateral trim procedure.
- The excess labia is removed, but the overall appearance of the vulva does not look as rejuvenated as with the other two procedures – there is a lot of wrinkling due to redundancy of the labia minora rather than a tight appearance.
- The design of the lateral trim resection does not allow the surgeon to include removal of excess clitoral hood, leaving a bulge resembling a small phallus (penis) at the top of the vulva in patients who present with very enlarged clitoral hooding.
- Removal of too much labia minora is not an infrequent complication.
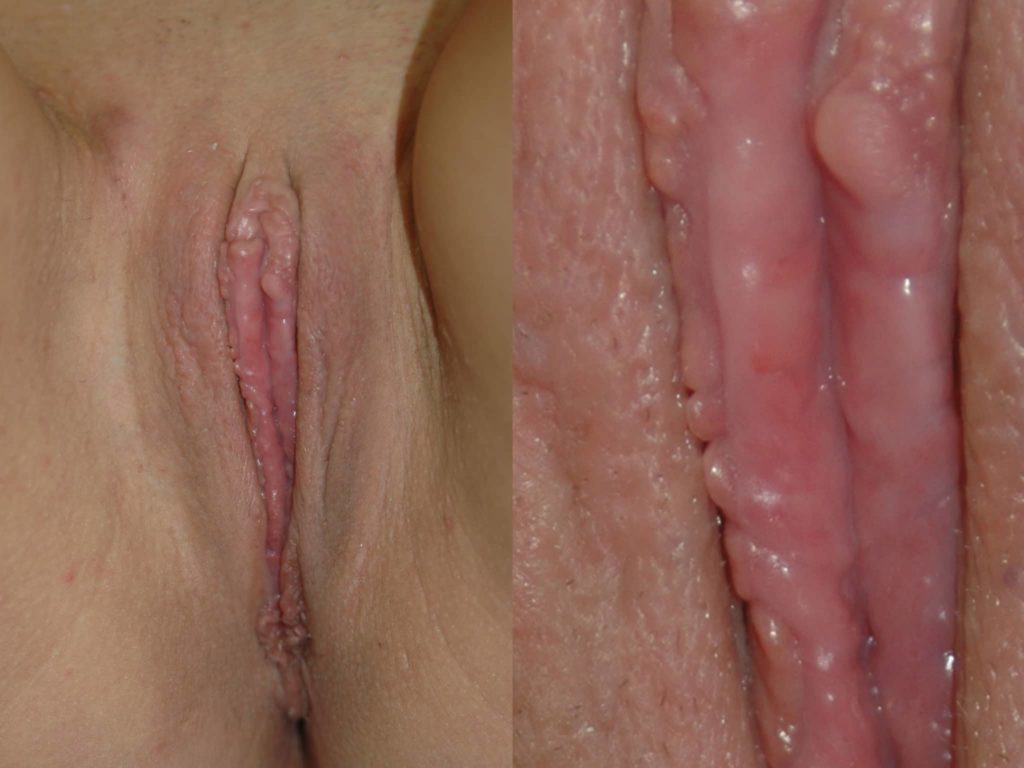
Left: Results after lateral trim labiaplasty.
Right: Close up view of the same patient showing “scalloping” (irregular edges) along the edge of the labia minora.
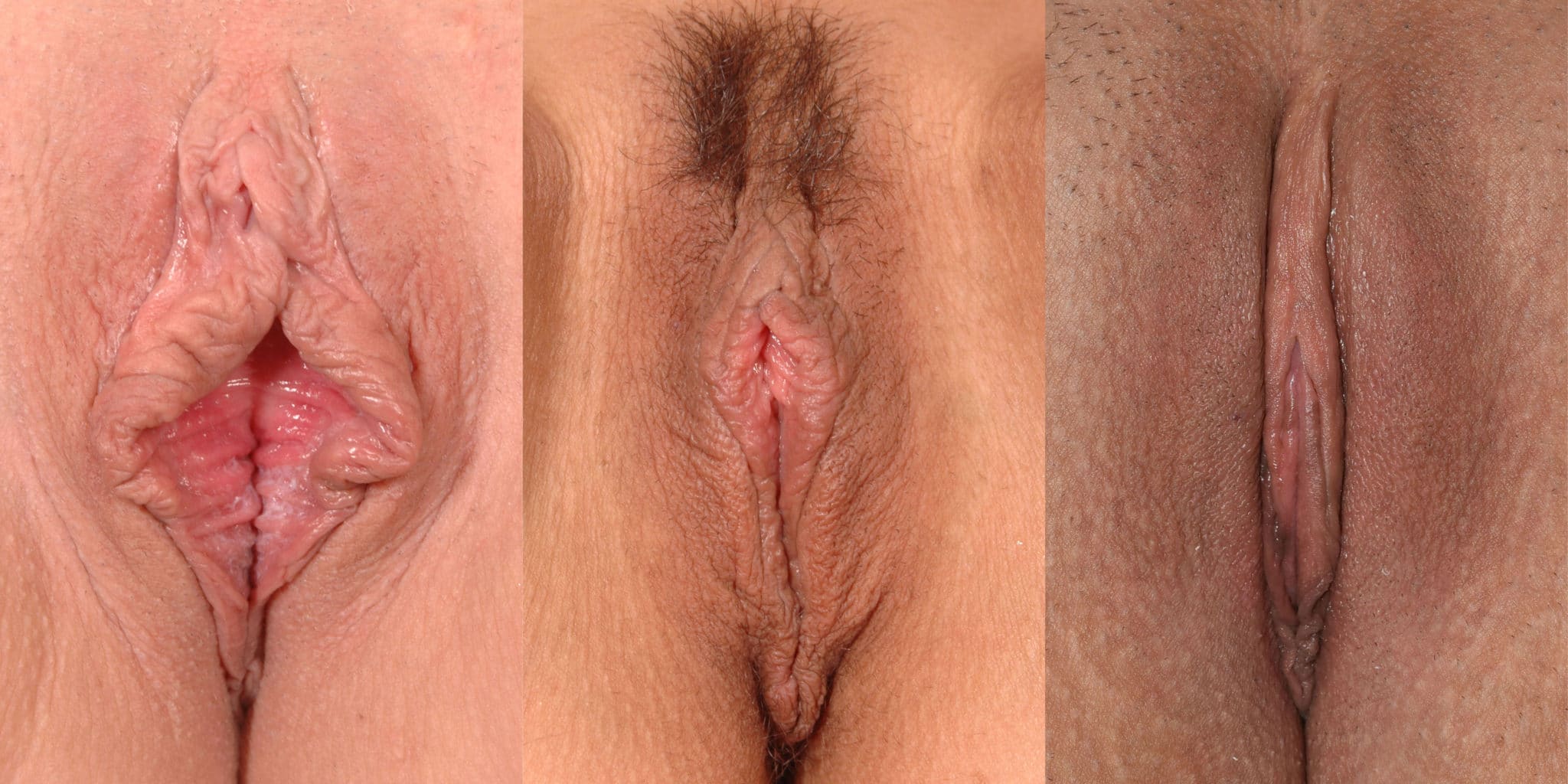
Left and Middle: Results after lateral trim labiaplasty. Note that there is severe wrinkling of the labia minora due to the fact that the vertical (height) excess of labia minora is not addressed by this technique.
Right: Results after central wedge resection labiaplasty. Note that the labia minora has been vertically tightened as well, leaving a much more youthful appearance overall. The age of the patient on the right is only three years younger than the patient on the left!
What are the Risks of Labiaplasty Surgery?
Though labiaplasty is considered to be a generally safe procedure, it is not without its risks. Risks of labial rejuvenation surgery include:
- Poor healing, fistula**
- Asymmetry
- Loss of labial sensation – probably theoretical. I have yet to see this in my practice.
- Infection – Extremely rare
- Bleeding – usually just minor wound oozing
- Unsatisfactory results – With central wedge and custom flask resections, I find this extremely rare! Lateral trim procedures often give cosmetically unsatisfactory results.
What is a Fistula?
A fistula is a small opening within the suture line causing a “window” in the labia minora. This results from breakdown in the suture line. This does not occur in the lateral trim because nothing but the edge of the labia minora is sutured. The proponents of this procedure hold out the risk of fistula as a reason to do only lateral trim. I have found that meticulous three layer closure, repairing the middle layer of the labia minora in addition to the inner and outer layers is absolutely essential to avoid fistula formation. In my practice, fistula formation occurs approximately 1 percent of the time, and is relatively simple to repair. In my opinion, the fear of a fistula occurring is not a valid reason to perform an inferior procedure (lateral trim).
In some cases, secondary surgery may be required to fix complications caused by the initial procedure. I review the potential risks and complications of labiaplasty prior to the surgery. Luckily, complications from labiaplasty are rare and there are options to treat these complications should they arise.
What Our Patients Have to Say
"I saw Dr. Epstein for labia reduction surgery (labiaplasty) in May of 2014. If you or someone you are close with is considering this surgery, Dr. Epstein is hands down the person to see. Having the surgery was something I knew I wanted done since I was a little girl, even before I knew labiaplasty existed. I spent years and countless hours searching online for doctors who not only did this surgery, but did so it was undetectable after healing. Dr. Epstein was an absolute god send and has truly changed my life."
“Dr. Epstein Is Just The Kindest Man And He Is An Exceptional Surgeon. His Staff Is Amazing As Well. Our Experience Could Not Have Been Better!”
The Labiaplasty Consultation
How Is Recovery After Labiaplasty Surgery?
At the end of the surgery, I place a long acting local anesthetic called Exparel. This results in a dramatic reduction of post-operative discomfort as well as the need for narcotic pain medication for the next several days. After surgery, the patient applies bacitracin ointment a few times a day to the area to prevent infection and scabbing. No bandages are necessary and there are no sutures to remove – everything dissolves! There is no other dressing other than a thick pad such as a maxi pad, or combine dressing for the first few days. There is no problem with toileting. The labia minora are fairly swollen for several days, but this resolves over the next few weeks*.
You can shower as soon as you wish, even the same day as your surgery! You can drive, go to school or work the next day if you feel up to it. You should not have intercourse, use tampons, ride horseback, a motorcycle or bicycle until six weeks. I will see you a day or two after surgery, at three, six and twelve weeks after surgery. Complication rates are very low. The most common one is a small area of wound separation. This heals spontaneously with no special care other than the application of bacitracin ointment or a very minor revision. This is performed under local anesthesia at no charge.
Labiaplasty Results
In my experience, patient satisfaction with labiaplasty has been very high using the Central Wedge or the Custom Flask labiaplasty techniques. Both of these procedures offer greater flexibility to sculpt the labia. They also address clitoral hooding, in which the external trimming technique does not permit. Furthermore, both techniques leave the natural labial edge on the outer border of the labia. As already discussed above, the external trimming technique leaves scar tissue along the outer edge of the labia*.
If you are interested in viewing my labiaplasty procedure before and after pictures, click here to view the labiaplasty gallery.
Schedule A Vaginal Rejuvenation Consultation
To learn more about labiaplasty (vaginal rejuvenation), contact the office of Dr. Mark Epstein. Call us at 631.689.1100 to schedule a consultation or you can fill out our online form. Our practice serves Long Island and surrounding areas in New York.



