The four main incision locations – advantages & disadvantages
Armpit (Transaxillary)
The incision is made in the armpit. The idea is not to have any scar on the breast. Usually, the pocket dissection is done blindly, which results in more bleeding around the implant after surgery. I have performed many such procedures, but I use an endoscopic approach where a video camera is inserted into the incision to guide the surgery. Dissection of the breast pocket is more precise than with a blind technique, and any bleeding that is identified can be dealt with immediately.
My personal observations are that the results with this technique are OK, but pocket dissection is not as precise as with other techniques, which makes the correction of asymmetric breasts more difficult, and achieving symmetry, especially when the lower breast creases are at different levels, is harder than with other approaches. Also, as there is more blunt dissection, a 24 hour recovery is not as likely. When I perform the surgery with saline implants (which are inserted deflated and rolled up like a cigar), I use a 2.5 cm incision (the width of my index finger). However, the manufacturers of silicone implants recommend a larger incision for those implants, so it would be difficult to hide a larger incision in the axilla. Also, it is much harder to remove the implant during surgery if a pocket adjustment is required. Therefore, it is not my preference to use a transaxillary approach for a silicone gel implant.
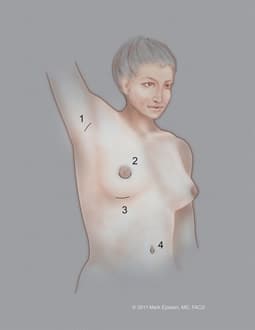
1. Armpit (Transaxillary) 2. Nipple (Periareolar) 3. Inframammary (Lower Breast Crease) 4. Transumbilical (Navel) ©2011 Mark Epstein, MD, FACS
This approach is also not indicated when a dual plane II or III technique is required for a type II breast with bottoming out of the glandular tissue, as the surgeon needs to come from the bottom upwards inside of the breast, not the other way around. Dual plane II and III cannot be performed adequately from a transaxillary approach.
There is an option to perform a breast augmentation in the preservation space through an armpit incision. This is called the MIA procedure and it is requires both specialized instrumentation and the Motiva Ergonomix2 implant. The implant sizes for this procedure are under 200 cc. Both the instrumentation and the Motiva Ergonomix2 implant are not yet available for use in the United States. It is my hope that as soon as these are available in the U.S., I will be able to offer the procedure here.
Nipple (Periareolar)
This approach involves making a semicircular incision around the areola (the pigmented skin around the nipple), usually on the lower half. With this approach it is possible to perform a dual plane II or III pocket dissection. The main advantage to this technique is having an inconspicuous scar around the nipple/areola complex. Not everyone heals the same. Some people heal with a hairline inconspicuous scar around the areola. Some people don’t. The surgeon and patient often times cannot predict who will heal with a less obvious scar and who will not. So, the main disadvantage is really the same as the advantage in reverse: if you heal with a very unsightly, visible scar, it is now on the most conspicuous part of the breast. The other issue to consider is that there is a 8-10x higher capsule contracture rate associated with this technique. There are microorganisms within the nipple ducts and these microorganisms may contaminate the implant during insertion or during creation of the implant pocket. This has been associated with the development of capsule contracture of the breast. This often results in the need for a second surgery to treat the capsule contracture. I have used this technique, but prefer the inframammary approach.
Inframammary (Lower Breast Crease)
This is the most popular approach. It gives direct exposure to the lower edge of the pectoralis muscle so that it may be elevated to place an implant under the muscle if so desired. It also gives the surgeon the very best view of the entire breast pocket, so that the pocket may be dissected as accurately as possible. Also, just before closure of the wounds, the surgeon can visualize the lower edge of each implant so as to make certain they are at the same level so the breasts look even in height. If a dual plane II or III approach (this will be explained later) is desired, this incision gives the surgeon the best exposure to do so. Another advantage is that when using this technique, I can then place a sterile, clear plastic adhesive dressing over the nipple to prevent any bacteria from inside the nipple ducts from contaminating the surgery and resulting in an increased risk for capsule contracture. This is one of the many steps I take during surgery to prevent capsule contracture. If I was using a periareolar (nipple) incision, I would not be able to do this.
Due to the unparalleled view of the breast pocket and ease of surgical dissection, this approach easily lends itself to a recovery in 24 hours. Some of the critics of this approach claim that the incision and resultant scar is often higher than the crease after surgery. Some surgeons even intentionally make the incision a little above the natural lower breast crease so that if the woman lifts her arms up when wearing a bathing suit, the scar won’t be exposed as the lower edge of the bathing suit top rides up. This is nonsense.
Here’s the real deal. If you want the scar to be an inconspicuous as possible, you want the scar to end up in the crease where it lays after surgery. This may involve making the incision actually lower than the natural breast crease. This is especially true in the type I breast, which is tight and perky. In these women, it is imperative to have the scar in the crease because the breast will most likely not have enough natural sag to fall over and cover the scar. With proper surgical planning, it is relatively easy to have the resultant scar fall within the new crease that forms after surgery so as to make the scar as inconspicuous as possible. When the scar lies within the crease itself, there is the least amount of tension acting on it, so the appearance of the scar is optimized. The more tension acting on the scar, the thicker it becomes and the more obvious it is. When the scar ends up on the lower portion of the breast, as opposed to within the actual breast crease, the scar is far less visible.
The incision for the Preserve breast augmentation procedure utilizes and incision in the breast crease.
Transumbilical (Navel)
I personally do not use this technique. It involves making a small incision around the upper portion of the belly button (navel) and inserting a balloon under the breast. In some cases it can be placed under the muscle, but in most cases the pocket is above the muscle. The balloon is inflated and bluntly separates the tissues apart. Also, for type II breasts requiring a dual plane procedure, this is not an option as a dual plane procedure cannot be performed through this approach. I am not in favor of this procedure especially in view of the fact that there are far superior procedures.
Prev Section: Pocket location – Above or below the muscle? »
Next Section: What would I like my recovery to be like? »
Sections – Five Key Decisions You Need To Make
Chapters – Breast Augmentation Guide
- Intro to Breast Augmentation
- Preservation Breast Augmentation – A New Era!
- Motiva Implants – What You Need to Know
- Five key decisions you need to make
- One-Day Recovery Breast Augmentation
- Anesthesia – General, Sedation or Local?
- Breast Lift (Mastopexy) with/without Implants or Fat
- What else should I know about breast augmentation?
- Important Things to Consider When You Decide to Move Forward With Breast Augmentation
- Revision of breast augmentation
- ALCL and Breast Implant Illness