Introduction
Surgery is not only about surgical technique, it is equally about decision making. Both of these are partially learned from others, and partially learned by experience. For the younger surgeon, it is definitely more of the former. For an older surgeon, like myself, it is definitely more of the latter. Surgery, just as in life in general, is all about understanding what we can control, and what we cannot control. For a typical surgery, you can make a list of these. Here is a list for a typical breast augmentation:
Things I can control during breast augmentation surgery:
- Incision length and location
- Implant pocket location (above/below muscle)
- Implant pocket size
- Implant size
- Use of betadine and antibiotic irrigation (to reduce risk of infection and capsule contracture)
- The method of pocket creation which will influence recovery (gentle electrocautery vs. blunt “rip and tear” dissection)
- The method I close the wound
Things I cannot control during breast augmentation surgery:
- Wound healing
- Tissue stretching and thinning
- Influence of gravity on the implant and breast tissues
One would look at this list and say “Wow, I sure have the majority of the control of the outcome of this operation!” My reply to that is “Wrong!” Let me go into a bit more detail:
Wound healing: By wound healing, most people think I am referring to the quality of the scar. While this is absolutely true, the quality of the mature (healing is completed) scar is only a small part of the process. Wound healing is a complex, only partially understood dynamic process that varies considerably among inidividuals. After a breast augmentation is performed, the surgical wound, specifically the incision in the skin, and the pathway down through the fat, to the muscle and ending at the pocket where the implant resides is healing by different processes and rates depending upon what tissues are uniting: muscle to muscle or fascia, fascia to fascia, fat to fat, skin to skin. For those curious, fascia is the thin layer of tough connective tissue that lines the surface of muscles and the underside of skin. This is the thin, but strong layer that holds sutures, allowing us to secure different tissues together. While the patient is focused only upon how the scar looks, much more is going on inside the breast.
Let’s also not forget one other minor detail. The implant is now sitting in a pocket. Before this space was a pocket, it was two layers of tissue that lay one above the other. The muscle and breast lie above, and the chest wall lies below (in the case of a submuscular augmentation). In the case of a subglandular augmentation, the breast lies above and the muscle and chest wall lies below. In either case, these new exposed planes of tissue are also healing. But healing to what? They certainly do not grow into and attach to the implant? What happens is that in the human body, anytime a foreign body is placed inside our body, be it a pacemaker, artificial joint, twig, bullet or a breast implant, the adjacent tissues react by encapsulating the foreign body with a layer of scar tissue. I would look at this as a self-defense mechanism somewhat akin to how an oyster creates a pearl around a piece of sand that enters its oral cavity. The question then becomes how thick is this scar tissue? What is the quality of this scar tissue? Why is this important if you do not see it?
The scar tissue that forms around a breast implant is typically very thin and pliable. It is inconsequential to the look and feel of the breast. That is a good thing. Sometimes, and for reasons only partially understood, this scar tissue thickens and actually contracts. As it contracts, it makes the implant feel firmer. There is no actual change in the implant, it just feels firmer. If you squeeze a water balloon in your hands, you can simulate this effect. Now we have a problem: the breast feels hard, looks rounder, and the implant even rides upwards on the chest. This is called a capsule contracture. Fortunately, this does not commonly occur. As we do understand some of the factors that cause capsule contracture to happen, there are definitely interventions done during surgery that have been proven to dramatically reduce the risk of this from happening, but unfortunately, we cannot eliminate that risk 100%. You can read more about capsule contracture, what causes it and how it is treated here.
Tissue stretching and thinning: This is conceptually a lot easier to understand than wound healing. Skin is living tissue. It is made up of, among other things, collagen and elastin which are proteins that give skin both strength and elasticity. Every elastic material, living or otherwise, has its limits. If you apply a force to an elastic material, it will deform in response to that force. Once that force is removed, the material will revert to its former dimensions. If you apply too great a force, and exceed the elastic limits of that material, then it can break down, and lose the ability to revert back to its former dimensions. This is especially true with skin and other living tissue. If an excessive force is applied, there is breakdown of the collagen and elastic matrix, resulting in permanent stretching of that tissue. The placement of a breast implant is essentially a deforming force on the breast tissues. The larger the implant, the greater the deforming force on the tissues. A smaller implant – small amount of force. A larger implant – a greater amount of force. Some tissue stretch to accommodate the implant is both desirable and expected. When I place an implant, there is almost always a distortion in the contour of the breast, at least initially. The breast is not used to accommodating that implant, so the tight lower breast tissue envelope pushes back against the implant, causing it to shift its contents (saline or silicone gel) upwards. This is what causes the “hump” that we observe after just about every breast augmentation. Then, over the next few months, the breast tissue stretches, and as the tissues now accommodate that implant, the implant itself can now have a more desirable distribution of its contents, resulting in the breast attaining a more pleasing contour. This is illustrated in the case below:
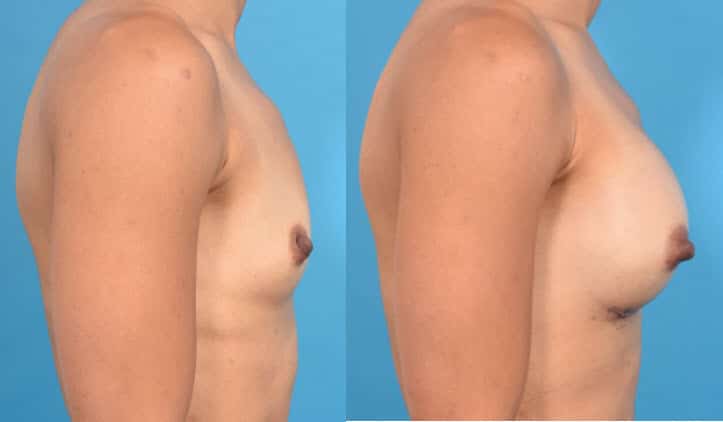
Pre Op 2 days Post Op
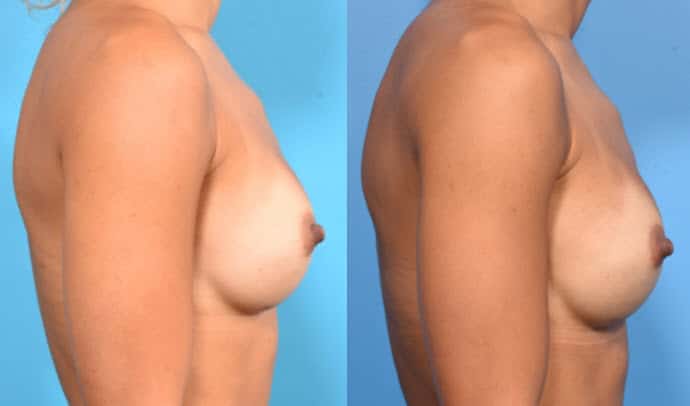
4 mos Post Op 1 yr Post Op
In the example above, before surgery, the patient has a small, tight breast, typical of a young woman who has yet to have children. Two days after surgery, the implant is exerting a force from inside the breast, causing some distortion. As the lower breast is very tight, the silicone gel is being shifted upwards, causing the “hump” or as we say, excess superior pole fullness (the superior pole is the upper breast). Note that the lower breast does not expand much at all compared to the upper breast. At 4 months after surgery, the breast tissue is now stretching in response to the implant and the force of gravity on the implant as well. The breast is now attaining a nice, pleasing shape. At one year, the breast has reached its final shape. The excess upper breast fullness is now completely gone, leaving a very natural slope from the upper chest wall to nipple. The lower breast crease has dropped a few millimeters, which is entirely normal and does not at all affect the aesthetic result.
If the implant is too large for the breast, then the amount of force exerted from within onto the breast tissues rises exponentially, causing severe stretching and thinning of tissues which can create a potentially uncorrectable deformity. Furthermore, the descent of the breast crease can become significant, resulting in a bottomed-out appearance to the breast. You can view examples of this as well as the result of its surgical correction here.
Gravity: While you cannot control or modify it, gravity is a known and constant force upon the breast and this implant that lies within. It can be your friend, or your foe, depending upon how you harness it. I plan my surgeries with this in mind. If you place an implant that fits the breast as described in the section about selecting implant size, then gravity will act as your friend, and provide the finishing touches on the breast to give the most natural possible result, as shown above. If you select an implant that is too large for the dimensions of the breast, or too heavy based upon the quality of the breast tissues (especially in post-partum women and revision cases), gravity will pay the price and you will permanently damage the tissues even further. This will result in an overly bottomed-out looking breast with loss of upper breast fullness. Surgical revision, if possible, will be the only option, will take more time than the primary (first time) augmentation and will also be more costly.
Putting It All Together
This all sounds very ominous. Is breast augmentation a crap-shoot? Certainly not! I have been performing this procedure for over twenty five years; my patients and I are very satisfied with the results. You can see numerous examples in the website photo gallery. The essence of all I have presented is this: while I cannot eliminate factors I cannot control when performing breast augmentation surgery, I have a thorough understanding as to how these factors can affect my surgery. I know that I have the power to minimize unpredictable, untoward results but I cannot eliminate them completely. I have been able to perform this surgery with a three year re-operation rate of approximately 2% versus a national average of 15-40%, depending upon the study you read.
How is it possible I achieve the results that I do? It is certainly not magic. I understand what factors cause unsatisfactory results in breast augmentation, and the biggest factor is usage of implants that are too large. That is why I use a tissue-based bio-dimensional approach in selecting the size of the implant. Nothing is 100% and nothing is 0%. There are those who tend to use much larger implants than I do and I am sure that they on occasion get away with it. I use a special approach to avoid problems. Does this work every time? Of course not! However, over the course of thousands of augmentations, my re-operation and complication rate is exceedingly low. So while we cannot eliminate the unsatisfactory breast augmentation, by thoroughly understanding these factors out of our control and using defined processes for implant selection and performance of breast augmentation surgery, it is possible to minimize problems and to produce very satisfactory outcomes in the vast majority of my patients.
Prev Section: Do breast implants need to be routinely changed? »
Next Section: Breast Augmentation and Lactation »
Sections – What Else Should I Know
- Breast Augmentation with Fat
- Will my breasts be symmetric?
- How far apart will my breasts be? Will I have cleavage?
- The truth about incision size
- Do breast implants need to be routinely changed?
- Things We Cannot Control: Wound healing, tissue stretch and gravity
- Breast Augmentation and Lactation
- Setting realistic expectations for your result
- Breast Implant Rupture – How To Know? – Are Routine MRI Scans Really Necessary?
- Mondor’s Cords – What Are They?
Prev Chapter: Breast Lift (Mastopexy) with/without Implants or Fat »
Next Chapter: Important Things to Consider When You Decide to Move Forward With Breast Augmentation »
Chapters – Breast Augmentation Guide
- Intro to Breast Augmentation
- Preservation Breast Augmentation – A New Era!
- Motiva Implants – What You Need to Know
- Five key decisions you need to make
- One-Day Recovery Breast Augmentation
- Anesthesia – General, Sedation or Local?
- Breast Lift (Mastopexy) with/without Implants or Fat
- What else should I know about breast augmentation?
- Important Things to Consider When You Decide to Move Forward With Breast Augmentation
- Revision of breast augmentation
- ALCL and Breast Implant Illness